 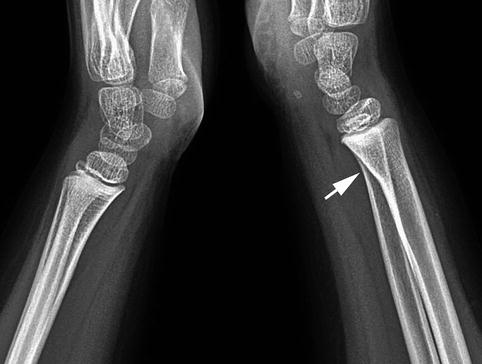
The proximal articular fractures are subdivided into avulsion, shearing, and multifragmentary fractures. The proximal metaphyseal fractures are extra-articular and segmented into transverse and oblique types. The AO Foundation divides the base fractures of the proximal phalanx into proximal metaphyseal and proximal articular. Unlike diaphyseal fractures, these do not tend to cause appreciable rotational deformity. This deformity tends to be maintained by the intrinsic muscle insertion on the base of the proximal phalanx (dorsal interossei) and the extension force of the central slip across the proximal interphalangeal (PIP) joint (palmar interossei and lumbricals insertion into lateral bands of the extensor hood). 1– 3 The fracture often results in a dorsal angulation at the fracture site in the base of the proximal phalanx. The trauma is most likely related to sports activities in the 10-to 30-year-olds, work related in the 30- to 70-year-olds, and due to fall from a standing position in people above 70 years of age. 16.1).Ī phalangeal fracture is the most common injury to the skeletal system and accounts for approximately 10% of all fractures. This type of fracture results in evident joint instability ( Fig. If coronal forces are applied to a finger, intra-articular avulsion fractures of the base of the proximal phalanx are a consequence of ligament strength superior to bone strength. A direct blow creating an axial load to the finger may result in a comminuted, intra-articular base fracture. An extra-articular transverse or oblique fracture is often the outcome of the described trauma, whereas torsion injuries might cause an oblique or spiral fracture of the shaft. Hyperextension and abduction of one of the fingers tend to cause a base fracture of the proximal phalanges, most frequently to the fourth or fifth finger. Keywords: conservative treatment, Buddy Loops, early mobilization Open reposition and internal plate fixation is a specialist procedure, where absolute stability is needed, so that immediate mobilization of the finger can be initiated soon after surgery. If osteosynthesis are required to maintain an acceptable position of the fracture after closed reduction, K-wire fixation should be considered, with respect for the anatomy of the extensor apparatus. Conservative treatment and immediate mobilization are first choice for undisplaced fractures. In this chapter, intervention options are reviewed focusing on restoration of finger function and to a lesser extent on exact reposition of the fractured digit. Treatment of base fractures in the proximal phalanx depends on the fracture type, the degree of displacement, and whether fracture reduction is stable or not. 16 Fractures at the Base of the Proximal Phalanx 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
